Lifelike Mannequins Prepare Nursing Graduate Students for Real-Life Emergencies
Last Updated on November 22, 2019 at 12:00 AM
Originally published November 22, 2019
By UC Staff
UTEP Communications
A 73-year-old car crash victim lies in the emergency room screaming "No me gusta!" or "I don't like it!" as students in UTEP's Adult/Gerontologic Acute Care Nurse Practitioners (AGACNP) program prepare to insert a tube into her trachea to help her breathe better.
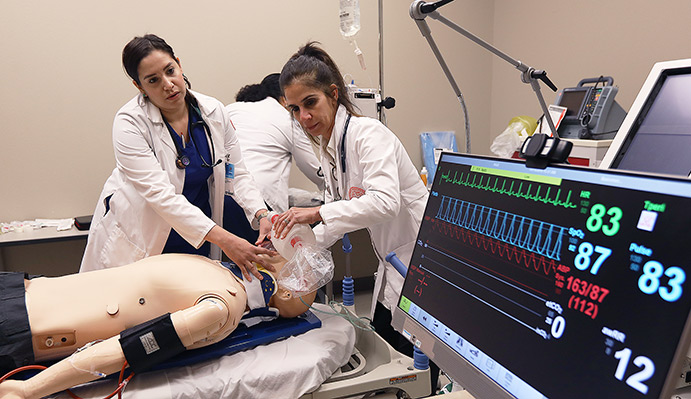
Students in the Master of Science in Nursing Adult/Gerontologic Acute Care Nurse Practitioners program practice their clinical and decision-making skills through various trauma scenarios in UTEP’s Center for Simulation using high-fidelity mannequins to simulate real-life emergency care situations. Video by UTEP Communications
The patient’s pulse is weak, her blood pressure is low and she’s bleeding from her arm and leg.
“I see on this FAST (Focused Assessment with Sonography for Trauma) exam, we do have some abdominal blood so she’s bleeding into her abdomen,” said Jill Shaw, the team’s leader, as she examined the patient’s ultrasound on the computer monitor. “Okay, let’s consult surgery.”
In trauma situations, the decisions that health care practitioners make can mean the difference between the life and death of a patient.
That is why The University of Texas at El Paso’s School of Nursing is using high-fidelity mannequins to simulate real-life emergency care situations.
Students such as Shaw in the school’s Master of Science in Nursing (MSN) AGACNP program practice their clinical and decision-making skills through various trauma scenarios in UTEP’s Center for Simulation without putting the patient in jeopardy.
The computerized mannequins mimic the body’s physiology. They speak, breathe, bleed and their chests rise up and down. The patient monitor also can provide an X-ray, ultrasound, CAT scan, MRI images and lab results.
“The point of the trauma simulations is that we can make the high-fidelity mannequins critically ill to the point of death and the students have to intervene,” said AGACNP program director Kathleen M. Cox, DNP. She said students learn how to do primary and secondary assessments, which enable health care practitioners to identify and treat life-threatening conditions in an efficient manner.
“This is a place that they can be safe, they can make mistakes and they can learn from those mistakes,” she said. “So when they go out into the critical care environment, they have already learned how to do those skills because they practiced on a simulated patient.”
UTEP’s AGACNP program educates nurse practitioners to respond to patients with critical life-threatening illnesses and injuries. Since 2013, more than 120 nurse practitioners have graduated from the program, the only one of its kind in the Paso del Norte region. The program is set to graduate 34 students this December, the largest class in the program’s history.
Although the program is online, students participate in simulation experiences on campus at least once a semester. During October’s simulation exercise, students were divided into teams of four and they participated in two different scenarios: one was a car crash victim and the other involved a 53-year-old man who fell 15 feet from a construction scaffold.
During the car crash scenario, students checked the patient’s vital signs as part of the ABCDE (airway, breathing, circulation, disability, exposure) primary assessment. They followed up with a head-to-toe assessment where they looked, listened and felt the entire body for injuries.
“I’m examining her back,” said Shaw, after she determined the patient’s pelvis was stable enough to turn her on her side. “No injuries, no wounds. Checking rectal tone. We have rectal tone … Prepare her for surgery.”
Shaw first used the technology as an undergraduate nursing student, but this experience was far more intense, she said.
“The simulation models that we used in my undergrad program do not have the computer capability that these do,” recalled Shaw, a nurse for 10 years. “These are able to breathe, they have pulses, they can respond appropriately. They’re miles away from what we used before. It’s like working on a real patient.”
To prepare students to always expect the unexpected in trauma situations, instructors surprised them by having the patient’s son burst through the door and throw himself on top of the patient, accidently pulling an intravenous line out of her arm.
“That really helped because that happens all the time,” said Mustafa Azimi, an intensive care unit nurse for five years. This was Azimi’s first time practicing on a high-fidelity mannequin.
“I was really shocked to see how UTEP was able to include sim technology to help us understand how to run certain codes or certain situations, and how to respond to the patient,” he said. “It was pretty realistic considering everything I’ve seen out in the field.”
After the exercise, students met with faculty members who had observed them on cameras in the sim lab’s control room.
They commended the team on their communication skills, but the group did make one fatal mistake. The students gave the patient vasopressors to raise her blood pressure, which they later learned would not have helped her condition because of the massive traumatic volume loss if she were a real patient.
“I learned a lot from the nurses in the simulation with me and from our educators,” Shaw said. “I learned something brand new about vasopressors and trauma, so I appreciate the lab completely.”
High-fidelity mannequins are just one tool that the School of Nursing uses in simulation-based education. Family nurse practitioner students practice their communication, physical assessment, and documentation skills through digital clinical experiences. Undergraduate students receive hands-on training in a safe environment during simulated Hospital Days.
“Students that want to be the best come to this program because they know simulation sets our program apart from other programs,” Cox said.